Ninety-five percent of healthcare organizations say that strong interoperability is key to successfully transitioning to value-based care, but 85 percent say current interoperability solutions are not meeting their needs.
For healthcare professionals, inadequate interoperability also means less than ideal access to comprehensive patient histories—a barrier to care coordination that can result in care gaps and duplications and/or overtreatment.
All of this comes with a risk to patient safety and outcomes—not to mention a massive cost to the U.S. healthcare system estimated at $148-226 billion annually, or $1.5-2.3 trillion over 10 years.
Given that there are an estimated 884.7 million physician office visits every year, it’s critical that the information from these visits, as well as care received in other settings like clinics or the emergency room, is accessible by everyone—every doctor, nurse and pharmacist—who is involved in a patient’s care. 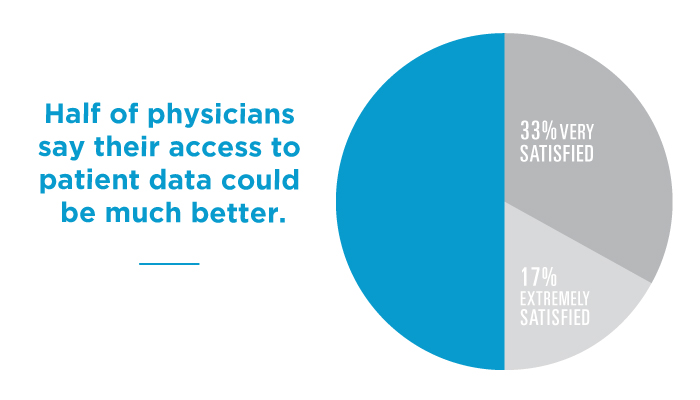
Half of physicians say that their access to patient data could be much better. This is according to a recent ORC International survey commissioned by Surescripts revealing that just 17 percent of physicians are “extremely satisfied” with their access to patient information, and just 33 percent are “very satisfied” with it.
This and other key findings are now available in our new report Physician Perspectives on Access to Patient Data.
The industry has experienced major progress toward interoperability in part due to ubiquitous electronic health record (EHR) utilization. EHR adoption has more than doubled since 2008 with nearly nine in 10 office-based physicians using and EHR by 2015. But while our survey was limited to only physicians using EHRs, the responses indicate that EHR utilization alone is no guarantee of adequate access to comprehensive patient information at the point of care.
Along with convenient access to patient data, 88 percent of physicians prioritize having patient history information, but only 30 percent can easily access it. This is a significant gap between how important this data is to physicians and the state of their ability to obtain it. Even the most basic details such as the names of a patient’s other care providers can be elusive. Just 33 percent of physicians can easily determine the other care providers their patient has seen, and only 30 percent can securely communicate with those providers electronically.

Since 2001, we’ve been building an industrial-strength health information network designed to increase patient safety, lower costs and improve quality of care. Today, the Surescripts Network Alliance® includes virtually all EHRs, pharmacy benefit managers (PBMs), pharmacies and clinicians, plus an increasing number of health plans, long-term and post-acute care and specialty pharmacy organizations who collectively:
- Transmit nearly 13 billion transactions a year, including nearly five million electronic prescriptions each day.
- Connect 1.3 million healthcare professionals
- Leverage a master patient index (MPI) of 230 million patients, or nearly the entire U.S. population
Our nationwide interoperable network delivers actionable patient intelligence directly to the EHR and enables physicians and other healthcare pros to make the safest and best-informed care decisions possible.
Using our Medication History solutions, physicians get a more complete picture of the care their patient has received from other providers. According to Surescripts internal network data, there were more than one billion medication history transactions in 2016.
For example, Medication History for Reconciliation covers 85 percent of U.S. patients, replaces a manual process that takes up to an hour per patient and enriches the patient-reported history by 28 percent, adding 1.1 drugs per patient that would otherwise be missed. Further, electronic medication reconciliation can prevent 35 percent of all admission medication history errors, 31 percent of the resulting inpatient order errors, 47 percent of most severe admission medication history errors and 61 percent of the resulting severe inpatient order errors.
Clinical Direct Messaging gives physicians and other healthcare providers a seamless and secure electronic means for communicating and coordinating care with the other members of a patient’s care team. According to Surescripts internal network data, the solution delivered nearly 26 million clinical messages in 2017—32 percent more than in 2016. Nearly 50,000 healthcare organizations are connected to the service with access to more than half a million validated directory addresses. Each month on average, Clinical Direct Messaging reports nearly 110,000 unique sending addresses and nearly 230,000 unique recipient addresses.
For clinical history, Surescripts Record Locator & Exchange lets healthcare providers quickly locate and access patient records from across all 50 states, regardless of care setting and EHR. Recently, The Surescripts Network Alliance expanded its reach to 40 health systems representing 295 hospitals across the country. This means that clinicians working in these hospitals have access to clinical records for patients who visit any connected health system—plus the 600,000 healthcare providers across 35,000 clinics and 1,250 hospitals included in Carequality. In 2017, more than 51,000 clinicians utilizing Surescripts Record Locator & Exchange located 26.4 million documents explaining where patients had previously received care. And they exchanged four million clinical records during the last three months of the year alone.
Physicians want to improve care quality and reduce costs for their patients. But their ability to do so relies on having convenient access to patient information, especially from other providers and organizations who share in their patients’ care. Improving their access and meeting their need for relevant, high-quality patient data requires powerful technologies that work together to inform care decisions with actionable patient intelligence—wherever and whenever it’s needed. The strength and experience of the Surescripts Network Alliance and Surescripts’ portfolio of solutions rise to meet healthcare professionals and their patients at every point on their healthcare journey.
To learn more about the state of physician access to and need for actionable patient intelligence, download the report Physician Perspectives on Access to Patient Data.


 Dean Riggott Photography
Surescripts
Dean Riggott Photography
Surescripts

