Software standards allow for the exchange of information in much the same way a common language allows a conversation. But in healthcare, existing standards have often fallen short of supporting seamless data mobility. That’s changing as the HL7 Fast Healthcare Interoperability Resources (FHIR) standard comes into its own.
Rooted in the use of open application programming interfaces (APIs) and internet-based information exchange frameworks, FHIR enables greater access to health care data and information. It features common secure web transports, industry standard security models, and an ecosystem that encourages thoughtful workflows. These workflows define not only the technical details of how an interaction might occur, but also how they should occur. This detail provides real compatibility and interoperability across different systems and organizations.
Moreover, healthcare’s software engineers—the very people who develop and implement new standards—love FHIR.
“FHIR is so easy to implement and it’s also flexible, which means new applications can be built quickly," says my colleague Tim McNeil, director of standards at Surescripts. “And if you’re assigned to suddenly start reporting on COVID-19 cases to a public health agency, you can use FHIR to do so. You can get your interface up and running a lot faster than in traditional software development."
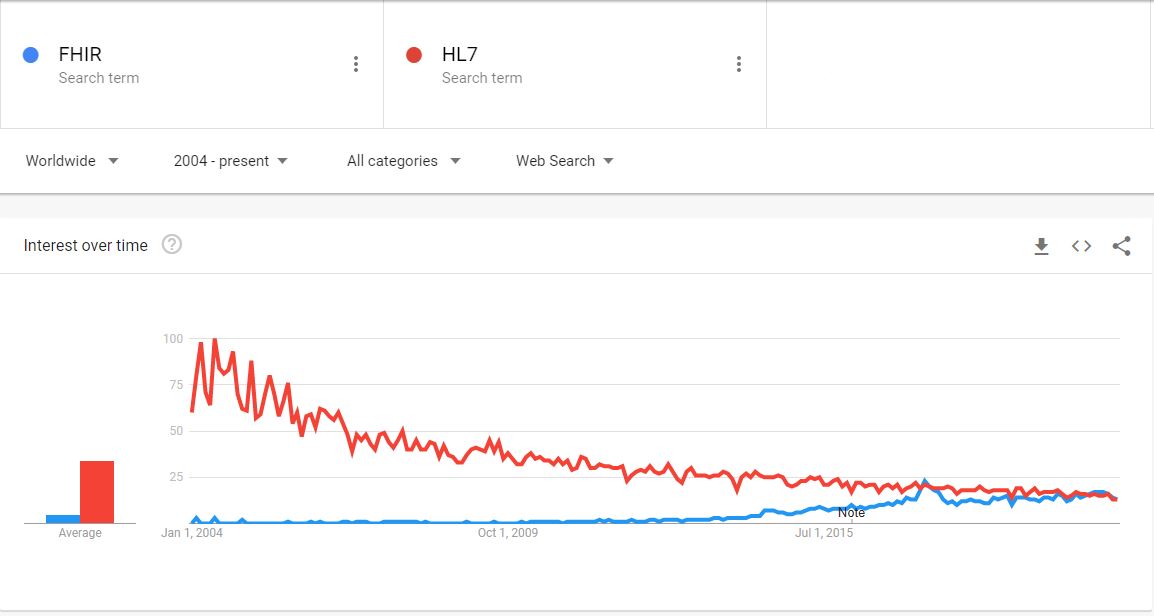
No wonder it’s catching up to traditional versions of the standard. FHIR only takes days to implement, whereas traditional standards can sometimes take months or years
Surescripts is part of two projects that have helped to develop and advance the adoption of this standard over the last several years: the Argonaut Project and the DaVinci Project. As such, we’re intimately aware of the power and promise of FHIR as we helped develop it, as well as its progenitor, HL7.
The standard forms a critical part of the Surescripts infrastructure and is a core component of several of our solutions, such as Record Locator & Exchange, Insights for Medication Adherence, Medication History for Populations and Specialty Patient Enrollment.
Surescripts is also part of the joint project between HL7 and the National Council for Prescription Drug Programs (NCPDP) to develop a FHIR implementation guide for specialty enrollment.
Spurred on by its ease of use and flexibility as well as continuous refinement, the number of solutions that rely on FHIR, as well as electronic health records software (EHRs) that have adopted it, has grown tremendously, especially in recent years.
Surescripts also performs the role of a sort of FHIR translator, says McNeil, which helps advance FHIR adoption while also allowing organizations to implement it on a timeline that works for them.
If one side of our network is using FHIR, but the other side is still using an older language or standard, we act as an intermediary and translate that language so that it can be consumed by the FHIR-supported application. This service pushes FHIR forward, without requiring its adoption by all stakeholders in order to work.
Critical mass for FHIR doesn’t seem far off, though, especially with federal requirements for its use serving as a catalyst.
The Office of the National Coordinator for Health Information Technology (ONC) has stated that FHIR is one of the important ‘tools in the toolbox’ needed to meet the interoperability goals in the 21st Century Cures Act. And both ONC and the Centers for Medicare & Medicaid Services (CMS) require support for FHIR as part of a new API certification process. Such initiatives and support are driving vendors to include FHIR support in their product offerings.
Both the DaVinci Project and the Argonaut Project have developed many use cases for FHIR, but looking to the immediate future, McNeil imagines it being used to monitor and notify providers about COVID-19 vaccinations.
There are a lot of potential FHIR-supported workflows specific to the COVID-19 vaccination, when and if it comes about. For example, the pharmacy administers the vaccine to a patient, and then there's a “FHIR call” to indicate it’s been administered, which is sent to a registry of immunizations, he says. We could also develop a FHIR-supported workflow to ensure that the patient’s primary care physician receives an EHR notification of the vaccination, or to ensure that the patient receives a booster shot, for example.
I asked McNeil what he thinks FHIR’s ideal future state should be. "We want the future to be more FHIR. We want FHIR to take hold across more parts of the healthcare ecosystem and accelerate the healthcare revolution, particularly greater information sharing and interoperability.”
I couldn’t have said it better.
Read on to learn more about how we’re working to advance information sharing across healthcare.


 Dean Riggott Photography
Surescripts
Dean Riggott Photography
Surescripts



