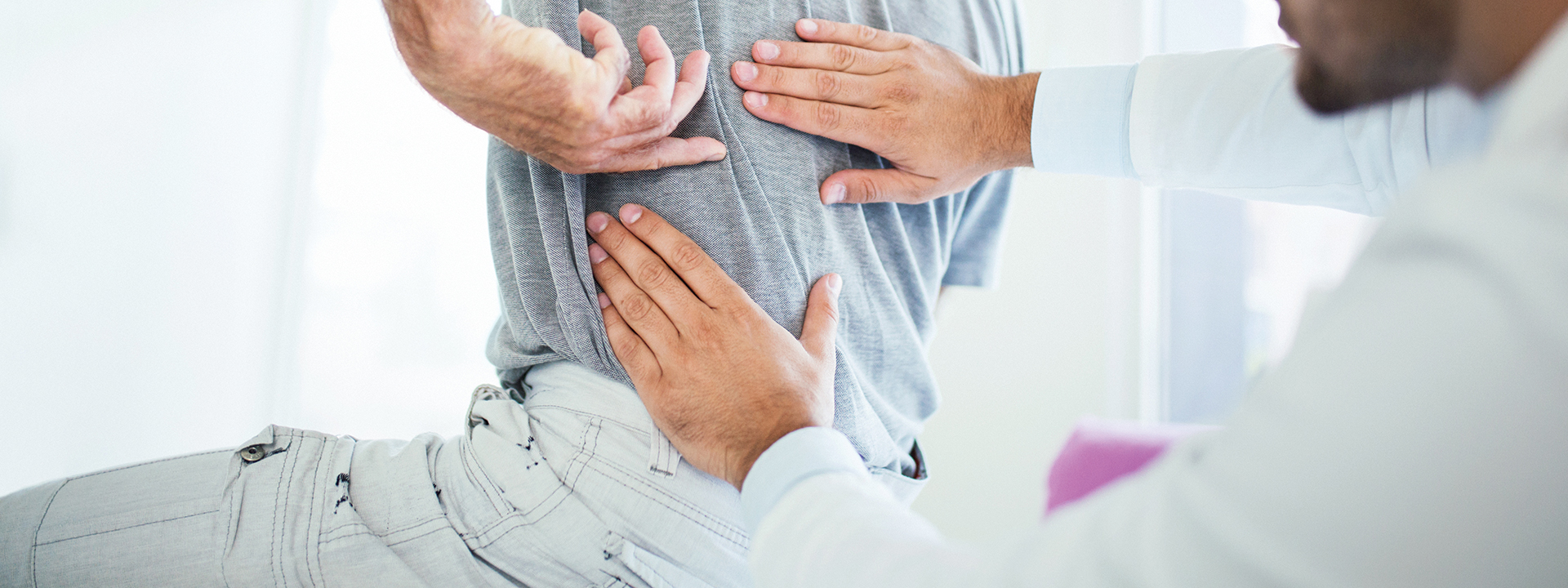
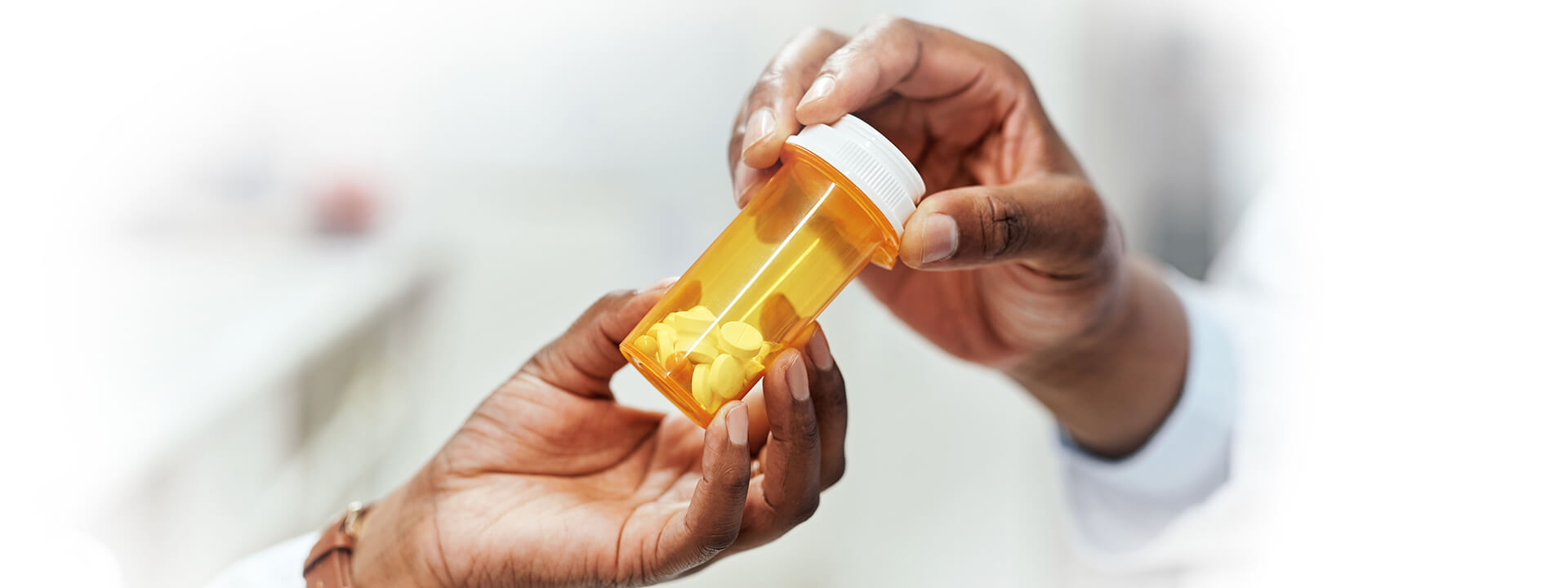
The opioid crisis has prompted stakeholders along the healthcare continuum to act. In 2016, the Centers for Disease Control (CDC) issued their guideline on opioid prescribing for chronic pain. I recently spoke with my colleague, Dr. Carol Forster, an expert in pharmacotherapy and chronic pain management and a consultant to the Drug Enforcement Agency, to discuss how the guideline will help prescribers deliver effective pain management in an environment fraught with risk.
“There’s a crisis. It’s claiming a record number of lives,” says Dr. Forster, Physician Director Emeritus, Pharmacy, Therapeutics and Medication Safety, Mid-Atlantic Kaiser Permanente Medical Group, and the Executive Director of Med Pharm Consulting, PLLC. “This federal guideline helps to ensure physicians are all on the same page when it comes to managing chronic pain and prescribing opioids safely and appropriately. It helps physicians do the right thing.”
The guideline covers three main areas: when to initiate or continue opioids; opioid selection, dosage, duration and discontinuation; and assessing risk and addressing abuse. The CDC has since followed up with a document that helps prescribers put the guideline into practice—and recommends using technology as a safe prescribing support.
“For those who prescribe non-pharmacologic and non-opioid therapies for pain first, then move to opioids as appropriate, the guideline validates their approach,” says Dr. Forster. “And for those physicians who weren’t aware of alternative therapies or were perhaps overprescribing opioids, this guideline was a sort of wake-up call. We now have physicians who are better educated and can manage their patients’ chronic pain in a safer and more effective way.”
As she explained, the guideline emphasizes that prescribers consider other pain management therapies before prescribing opioids. And if a prescriber does choose an opioid therapy for her patient, the CDC offers best practices for safer prescribing.
For instance, the guideline gives prescribers specific dosing guardrails: use caution when prescribing doses equal to or greater than 50 morphine milligram equivalents (MME) a day, and avoid increasing doses to 90 MME a day when treating non-malignant chronic pain.
These dosing guardrails seem simple enough. In truth, following them and other parts of the guideline can be quite complex. And per the CDC, prescribers need to implement the guideline with care, to ensure that they are not inadvertently putting patients at risk through an overly-rigid application of the guideline.
An MME Primer
MMEs standardize the total amount of opioids a patient is receiving to an overall dosage of morphine. This system is particularly valuable when patients are on multiple, different opioids.
To begin, a prescriber needs to know the patient’s medication history, including all the opioids a patient may take on a daily basis and at what dose. Then, the prescriber converts each dose to MMEs, adding them together if the patient takes multiple opioids. Based on this total number, the prescriber determines if the dosage falls within the CDC MME dosing recommendation. Next, she must determine how much she can prescribe or de-prescribe, all while balancing the patient’s reported responsiveness and pain treatment efficacy.
And that’s just the math! Let’s not forget that prescribers have to consider numerous patient-specific factors and clinical data points, such as medication tolerability and potential side effects.
The Case for Patient-Specific Data in Clinical Decision Support
Making sure a patient is on an optimal pain management therapy is onerous, but necessary. Clinical decision support (CDS) tools within the prescriber’s electronic health record (EHR) software can prove essential, especially when putting the guideline into practice. If used properly they can lift some of the burden, helping clinicians make more informed decisions. If poorly implemented, however, they can increase administrative burden or lead to less optimal pain management.
Ideally, CDS information should be embedded into the prescriber’s workflow and displayed at the right time without disruptive detours to other screens or applications. It must be meaningful and relevant. And, in the case of opioid prescribing, it must be based on a patient’s complete and accurate medication history.
Complete and accurate medication history data allows EHRs and technology vendors to create end-user clinical tools that help prescribers evaluate patient risk.
For example, patient-specific medication history enables the prescriber to see if the patient is at risk for an adverse drug event, if they are opioid naïve (which should prompt a lower starting dose) or if they are on multiple opioids and their MME exceeds the guideline. This data will also show if the patient has tried a non-opioid pain therapy, which the guideline suggests be the first choice in pain management.
“Medication history is a very important thing to have—and especially in this scenario,” says Dr. Forster. “A prescriber needs to consider compliance, and the patient’s entire regimen. You also want to check for other prescriptions that a patient may not have disclosed. Especially if you sense the patient may be drug-seeking and visiting ERs and other prescribers.”
Today, prescribers can access medication history data for nearly all Americans. This is impressive, but we know there’s still room to improve this service. And the opioid epidemic demands that we take every step and use every tool to rein it in. Medication history, as part of a clinical decision support toolkit, can help prescribers take the CDC guideline from abstract to actual practice. This is good news--for patients, for prescribers, for all of us working to rout this terrible epidemic.
To learn more how health information technology can help curb the opioid epidemic, check out our blog, Intelligence in Action.


 Dean Riggott Photography
Surescripts
Dean Riggott Photography
Surescripts