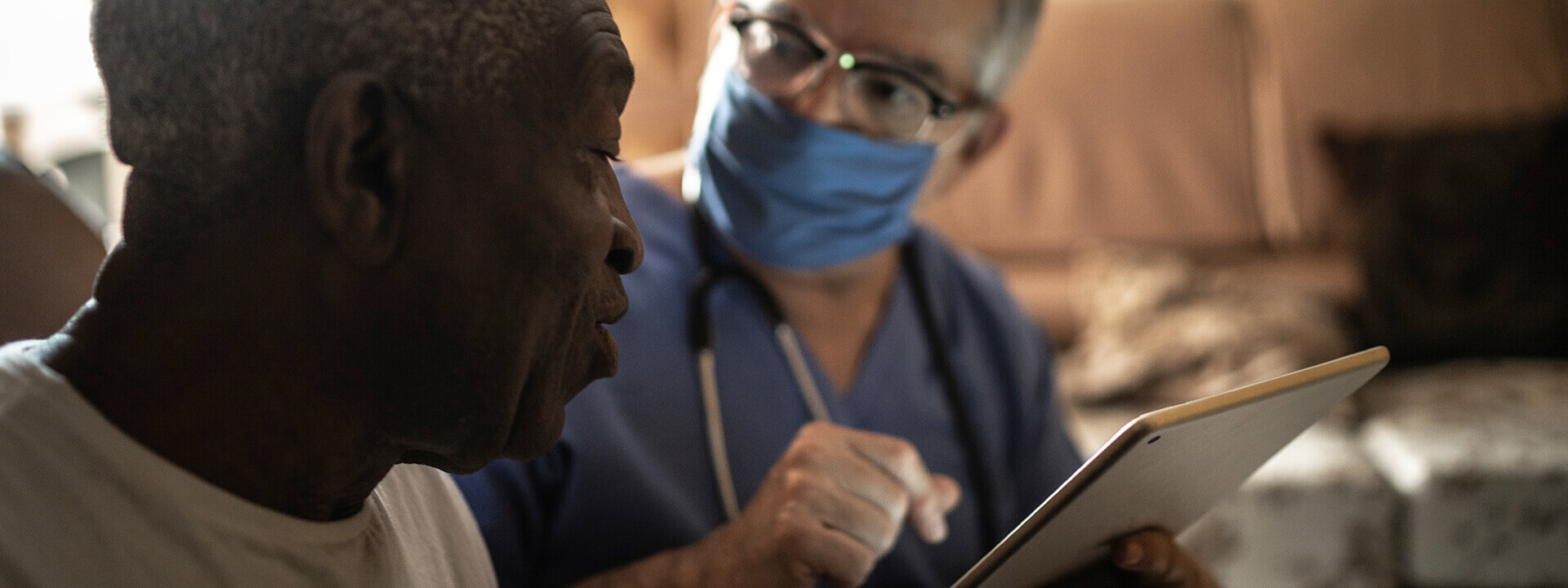
At the end of 2020, Congress passed legislation intended to drive greater price transparency for prescription medication. Part D Medicare plans are now required to implement at least one real-time benefit tool integrated into prescribers' e-prescribing and electronic health record (EHR) systems. And, starting January 1, 2022, qualified EHR systems under the ONC Health IT Certification Program must include a real-time benefit tool that conveys patient-specific cost and coverage information.
Both regulatory mandates are an obvious win for patients who are increasingly concerned about rising medication costs. These changes will accelerate the adoption of price transparency tools at the point of care and ultimately lower beneficiary costs.
But what's the benefit for physicians and health plans?
For prescribers, real-time benefit tools can minimize workflow disruptions and fundamentally change patient interactions. Having cost conversations at the point of prescriber can substantially increase medication adherence, patient satisfaction and patients' likelihood of staying with that provider. We surveyed U.S. patients, and over a quarter of millennials said they would be willing to find a new doctor based on whether or not that physician could have a medication cost conversation with them.
For health plans, in addition to the ways it empowers clinicians in-network, prescription price transparency tools can save commercial health plans $795 million and the commercial healthcare industry as a whole $3.7 billion annually.
To comply with these new regulations and laws, health plans and EHRs will need to choose a real-time benefit tool. It's important to find a real-time benefit tool that offers accurate and reliable data, integrates with existing e-prescribing workflows and has broad adoption among EHRs, pharmacy benefit managers and pharmacies.
Surescripts Real-Time Prescription Benefit is embedded in prescribers' existing EHR software and meets CMS requirements. It offers accurate, up-to-date prescription price and authorization information straight from the source: the patient's prescription benefit plan. And Surescripts’ Network Integrity Framework continuously protects and improves the privacy, security and quality of the network and the data it carries. In fact, Surescripts processes hundreds of millions of patient benefit checks at the point of care each year.
Surescripts applauds this legislation, and we believe it will improve patient care and their financial experience, but it's only part of the equation. Educating frontline care providers on the importance of using these tools—and how they can help them initiate crucial cost conversations with their patients—remains an equally important priority.
"I've been involved in health IT for 20 years now, and adoption and change is really difficult," Surescripts Chief Medical Information Officer Andrew Mellin, M.D., M.B.A., recently shared on an MGMA podcast. "A number of doctors have said this is one of the best clinical decision support tools they've ever had in their EHR. But there's still a large number of physicians who aren't eager to do something else in the exam room – because they're not aware the capability exists, they're worried it's going to take more time, or they don't feel like it's their responsibility. What's really important as a practice leader is making sure they understand the value of this. I think the biggest thing is don't expect just to flip the switch and have 100% adoption. To really see the value and benefit, it should be a systemic effort."
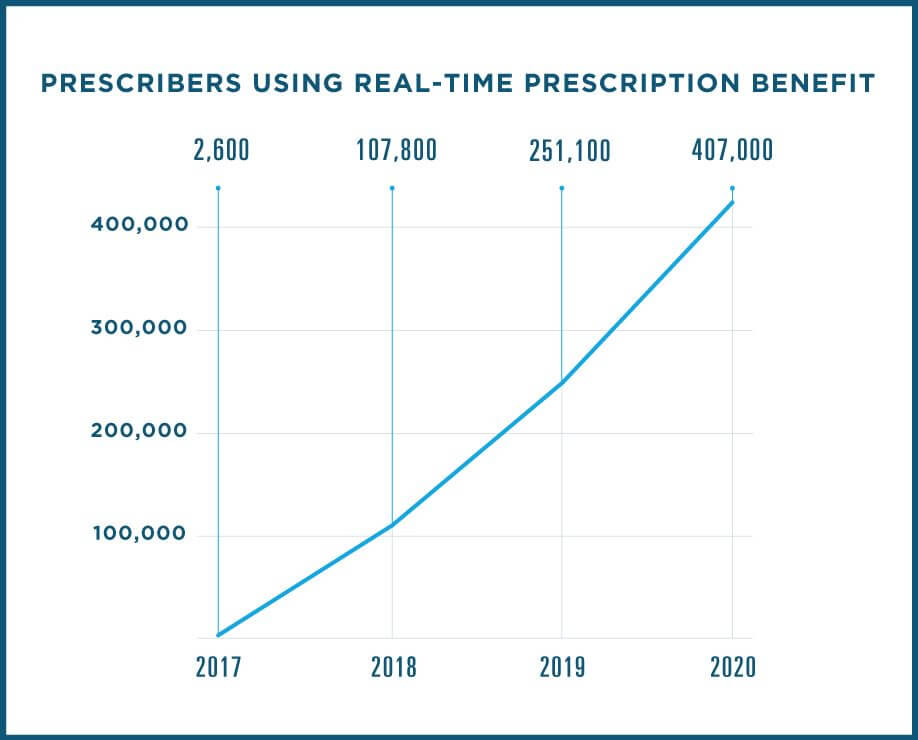
Legislation and education are making a big difference in the adoption of this tool. Today, over 88% of U.S. prescribers are served by an EHR with this feature or will have it soon. In fact, in 2020 more than 400,000 prescribers used Real-Time Prescription Benefit at the point of prescribing.
Listen to the MGMA podcast to hear more of Andrew's insights or learn more about Surescripts' Surescripts' Real-Time Prescription Benefit service today.


 Dean Riggott Photography
Surescripts
Dean Riggott Photography
Surescripts