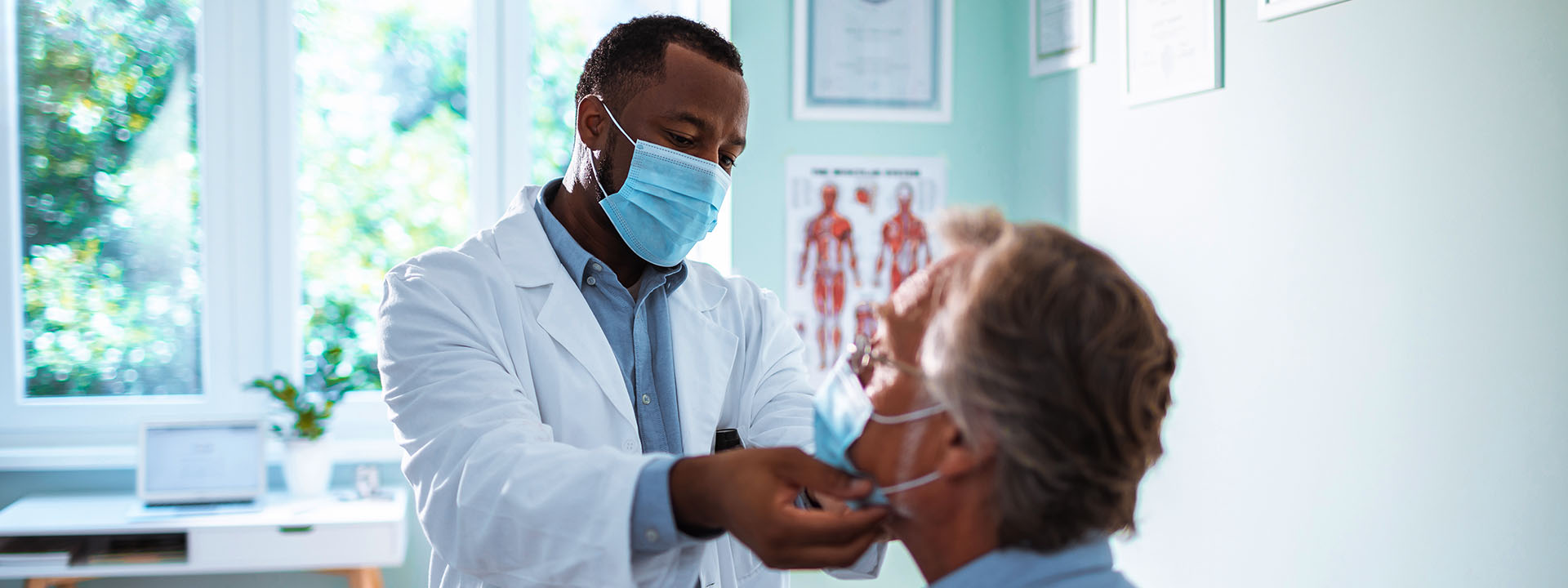
Care management has long been a top priority for providers and payers, but COVID-19 has shown us that we can't wait to realize the full promise of patient-centered and team-based care management. With COVID-19 long haulers, increased fragmentation in care delivery and delays in care during the pandemic, care managers will play an essential role in supporting the health of patients and removing barriers to care as we exit the pandemic.
These new developments coupled with other trends—increasing rates of chronic conditions and an aging U.S. population—all but guarantee a continued rise in healthcare costs. Organizations across the healthcare industry need to accelerate efforts to manage care to reduce per capita costs while improving the health of the populations they serve.
I spoke to Surescripts Vice President and Chief Medical Information Officer Andrew Mellin, MD, MBA, about the growing momentum for care management and how interoperability is helping meet today's care management needs.
-
Q: The Surescripts 2020 National Progress Report showed some remarkable progress with care management. What is your takeaway from these findings?
A: Two things stand out to me. The first is that the growing adoption of health interoperability tools means that care teams are gaining a clearer picture of patients and populations. In 2020 alone, more than 137,000 clinicians used Record Locator & Exchange to access and share patient records, including 426 million links to clinical document sources.
The second is that these adoption statistics also show that healthcare organizations increasingly recognize interoperability as a crucial component for well-coordinated care management. Solutions like the ones that Surescripts provides streamline access to information and eliminate friction and interruptions at many points throughout the care management workflow. But I should mention that interoperable technology is about more than just exchanging information; it's about exchanging actionable insights so providers can make better care decisions for patients.
Q: How do you get these types of insights?
A: When data is siloed, it makes information hard to get and often even harder to interpret. As a result, the everyday work of care management becomes slow and costly—and organizations miss out on the full potential of these programs. To fulfill the potential of care management programs, care teams need to tune out the noise and bring timely patient insights into focus.
Actionable insights are created when care teams have in-the-moment visibility into gaps in care, medication activity and patient care interactions. This information allows care teams to have more power to control costs and improve the quality of care.
Q: Can you share an example of actionable intelligence that helps providers make better decisions?
A: As COVID-19 reshaped how and who received care, we saw a critical need to deliver patient and population-level clinical and medication data. With access to actionable intelligence for 324 million patients, the care team can always review a patient's most up-to-date medication history, whether the visit is at a primary care provider, a telehealth provider, or an acute care provider.
And now, with Medication History for Populations, care managers can view medication history at a population level in between visits to identify patients with gaps in care and medication associated risks. In 2020, there was a 159% increase in the number of medication histories delivered to health systems, hospitals and accountable care organizations as part of their population health initiatives.
Read This
The Power of a Panoramic View of Patient Medication History
-
Q: Why is a network approach to care management important?
A: A network approach to care management is the only way to ensure a constant state of improvement and a steady stream of up-to-date patient data. By participating in the Surescripts Network Alliance, care management teams and healthcare organizations unlock access to critical clinical and medication data that help address costly—but common—gaps in care and coordinate successful care transitions. When they connect to the Surescripts nationwide network, care management teams within health plans and health systems get more timely patient insights to better coordinate care.
And the Surescripts Network helps each other. For example, pharmacists play an important role in managing complex medication regimens at retail pharmacies and health systems. Pharmacies also contribute prescription fill data to Medication History for Populations, which helps providers and physician-led network of accountable care organizations (ACO) like Aledade. Through Medication History for Populations, Aledade increased its star ratings for key quality measures and improved provider engagement.
Read This
How Aledade Improved Its Star Ratings With Enhanced Medication History
-
Q: Are there any other tools that you think are promising for supporting care management?
A: Tools like Record Locator & Exchange leverages the Carequality framework so that healthcare providers and organizations can quickly see where patients have received care and locate medical records, regardless of care setting and EHR. In 2020, more than 137,000 clinicians from 23,414 organizations, spanning all 50 states and Washington, D.C., used this tool to gain actionable intelligence.
Surescripts Insights for Medication Adherence helps clinicians identify adherence issues and gaps in care with patient-specific medication summaries and real-time messages from PBMs and health plans. We saw a 117% increase in clinical interventions supported by Insights for Medication Adherence in 2020.
Finally, RxChange streamlines communication between prescribers and pharmacists by making it easy for the pharmacist to suggest an alternative or start prior authorization, which can be completed within the EHR. In 2020, we saw a 30% jump in pharmacy enablement for RxChange and a 99% increase in RxChange requests.
By partnering with Surescripts, technology vendors can help give care teams a panoramic view of patients' health with timely insights from their clinical records and medication history. This allows them to spend less time tracking down information and remain focused on ensuring appropriate, timely and cost-effective care.
Visit Intelligence In Action to gain more insights on the role of interoperability and improved information sharing to meeting today's care management needs.


 Dean Riggott Photography
Surescripts
Dean Riggott Photography
Surescripts